Find information on GEMI Member Activities and other BC-Global Projects
Friends of Honduran Children Medical Brigades (FoHC)
FoHC is an NGO based out of Peterborough, Ontario with a partner NGO in Honduras. In 1998, Hurricane Mitch weakened the healthcare system, leaving up to 30% of the population without regular access to healthcare. FoHC and other NGOs provided relief in the Mitch aftermath, and have remained active in Honduras.
Each year, FoHC brigades travel to Honduras to provide medical, educational and construction support to communities in need identified by in-country logistics staff. Brigades are teams of approximately twenty made up of doctors, nurses, students and dentists. Brigades travel to remote villages with limited access to health care, establishing self-supporting medical clinics, dental clinics and pharmacies.
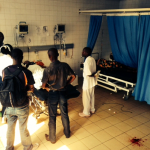
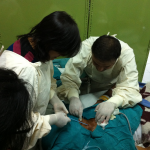
In February 2014, I joined a brigade (my fourth) to La Mosquitia, an area in northeastern Honduras only accessible to the mainland by air. Several villages are accessible only by boat: daily loading and unloading of approximately twenty-five hockey bags of supplies was a major undertaking! The local Miskito dialect required a Miskito to Spanish and then Spanish to English translation. Many villages had the poorest living standard I have experienced in Honduras to date; some children had no clothes to wear. The marshy landscape and insects contributed to many severe dermatological presentations.
The brigade provided primary and dental care for approximately 1200 patients. Our pharmacy distributed medications such as analgesics, antibiotics, vitamins, mass parasitic treatment, anti-scabicides and a limited number of food packs. We provided education regarding nutrition, pre-natal care, breast-feeding and safe water. We made arrangements for follow-up appointments for the sickest patients we saw.
Traveling to Honduras with the brigade is an experience I thoroughly enjoy. It allows me to give back and appreciate what we have here in Canada. Each brigade debriefs daily and upon returning home to discuss the work we do and where we can improve. I hope we can continue to be beneficial and have an impact for years to come.
Below is a picture of myself and clinic day crowds waiting to register.
Emergency Medicine Training in Rwanda
The first emergency medicine residency training program in Rwanda started in September 2013. This is a hybrid program where the first 12 months of training comprise a Post-Graduate Diploma course in “emergency medicine and critical care” (EMCC). All PGD residents are general practitioners who have completed six years of medical school and a two-year general internship. There are currently 11 residents enrolled in the PGD EMCC program. At the end of the 12 months of training, five residents will be selected to continue three additional years of emergency medicine training. Upon program graduation, they will receive a MSc in Emergency Medicine designation. PGD graduates will will focus their enhanced skills in emergency medicine to improve the quality of emergency medicine at the district level. M.Sc in Emergency Medicine are expected to run the tertiary care ED as well as the nascent residency training program.
This program is supported by the Rwandan Ministry of Health through the Human Resources for Health (HRH) initiative. http://hrhconsortium.moh.gov.rw/
A consortium of US universities supports HRH. The HRH universities supporting the emergency medicine training in Rwanda are Brown and Columbia Universities.
I am one of four foreign faculty that are delivering the EMCC clinical and didactic content. It is an exciting project with many challenges, frustrations, and hopefully, many meaningful outcomes.
Haiti-Project Medishare
http://www.projectmedishare.org
Through the hard work and dedication of Project Medishare, Hospital Bernard Mevs was established in Port-Au-Prince in 2010, five months following the Earthquake. It is Haiti’s only trauma and critical care hospital. One of the goals of Project Medishare is to recruit volunteers in order to mentor and train Haitian medical staff. Since its inception, over 5,500 health care professionals have volunteered their time.
I was fortunate enough to spend some time there in December of 2013. It really was a very memorable and significant experience for me. The people were welcoming and warm, the medicine was challenging and emotional, the weather was hot and the sleep limited.
In the broader context of global emergency medicine, the experience has some aspects that may not be for everyone. New groups of volunteers arrive every week; and it is hard to imagine how this process is not somewhat disruptive to the continuity of care and establishment of independent Haitian medical practitioners. It is also a private hospital and although there is a clear rational behind this, with respect to the long-term success and sustainability of this care facility, it doesn’t make it any less difficult to have to alter patient care based on financial restraints (coming from Canada, of course).
That being said, I am a full time ED doc who has two kids and who also wants to participate in and contribute to global medicine. This is not always an easy balance to achieve. Project Medishare provides a well-organized opportunity to volunteer one’s time, no matter how much or little of it you have to spare, in a place where your help is truly needed and appreciated.
GEMI is excited to formally announce its support of a new Emergency Medicine Fellowship in Lalitpur, Nepal. The Patan Academy of Health Sciences (PAHS) began one of the nation’s first post-graduate EM programs in September 2013. While most agree that GPs will continue to meet the acute care needs of rural Nepal, physician leaders in Nepal have seen the need to create a cadre of urban physicians with the expertise to develop emergency medical systems and the discipline of EM. The Fellowship in Emergency Medicine (FEM) at PAHS supplements the EM knowledge and skills of GPs who currently deliver emergency care so that they can become teaching faculty of EM Fellowship programs and future EM residencies.
The FEM is an 18-month program supported by emergency medicine educators and physicians from Canada. GEMI members can participate in this sustainable EM development initiative by visiting for a minimum of four weeks and volunteering their time to mentor Nepali physicians in the core concepts of EM. As “expert coaches,” visiting faculty help with formal learning such as journal clubs and core content review sessions, but they deliver their real value will by fostering fellows’ clinical learning and life-long learning skills. By role-modeling an EP’s role and by coaching colleagues, visiting faculty can play an important part in developing future EM leaders for Nepal. To date, Drs. Afshin Khazei and Sophie Low-Beer have enjoyed this rewarding experience, with many more GEMI members scheduled for 2014.
GEMI members who are interested in becoming involved with the PAHS FEM can download the “International EM Faculty for Nepal” document and/or can contact the GEMI executive committee members or Dr. Darren Nichols, International Faculty Coordinator, at dnichols@ualberta.ca.